Issues Addressed
WEIGHT MANAGEMENT:
Intervention Techniques: From among multiple successful drug-free approaches, we select those geared to the needs of the individual.
- Issues Addressed:
- Diet
- Supplements
- Exercise
- Motivation
- Procrastination
- Reinforcement
- Punishment
- Relationship Issues
- Reactions to verbal taunts
- Medical and medication complications
- Intervention Techniques:
- CBT REBT
- Hypnotherapy
- Reiki Healing
- Guided Imagery
- EMDR, EFT, Acupressure
- Meditation and Mindfulness
- Biofeedback
- Desensitization
- ...And More

EATING DISORDERS:
Dr. Gildston: Professional Member: Academy for Eating Disorders, National Eating Disorders Association, National Association of Anorexia Nervosa & Associated Disorders, Binge Eating Disorder Association.
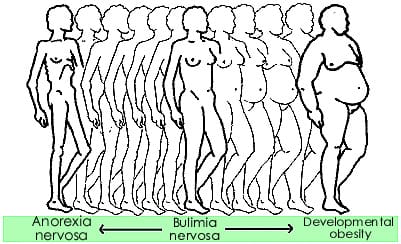
- Intervention Techniques:
- We have developed our own techniques to counter these serious problems, tailoring them to fit individual needs.
- All techniques are 100% drug-free.
- Challenges:
- Anorexia
- Bulimia
- Pathological Binging
- Body Dysmorphic Disorder (BDD)
- Developmental Obesity
-
- Mixed Categories
- Co-Morbidities:
- Substance Abuse Addictions
- Overindulgence in laxatives
- Alcohol and drug dependencies
- Depression
- Substance Abuse Addictions
-
-
- Anxiety
- Addictions and Compulsive Behaviors
- Purging
- Exercising excessively
- …and more
-
Our Director, Dr. Gildston:
- Presented recently an advanced professional workshop on Eating Disorders at the annual meeting of NYSCH.
- Was scheduled to present a workshop entitled “Why integrative psychotherapy is the way to go for addictive eating disorders” at the Annual Meeting of the Society for the Exploration of Integrative Psychotherapy.
- Presented a workshop entitled “Eating Disorders and Substance Abuse: Prevention and treatment for a spectrum of artful and dangerous addictions” at the Annual Conference of the NAADAC.
- Dr Gildston is also the director of A North Shore Center for Eating Disorders.
CHRONIC PAIN MANAGEMENT:
Dr. Gildston: Professional Member and Diplomate, American Academy of Pain Management
We understand the psychological toll of chronic pain. We also know that research studies indicate:
- Pain is felt in the body but controlled in the brain.
- The mind can be taught to increase the production of natural pain inhibitors. This faculty of the mind may allow for a decrease in the dosage of pain medications or may reduce the need for such medications altogether.

- Challenges:
- Headaches
- Migraine
- Tension
- Cluster
- Sinus
- Hormone
- Stress
- Headaches
-
- Back, Limb, & Chest Pain
- Fibromyalgia
- TMJ
- Carpal Tunnel
- Arthritis
- Irritable Bowel Syndrome
- ...And More
- Intervention Techniques:
- CBT REBT
- Hypnotherapy
- Reiki Healing
- Guided Imagery
- EMDR, EFT, Acupressure
- Meditation and Mindfulness
- Biofeedback
- Desensitization
- ...And More
Our Director, Dr. Gildston:
- Recently moderated a day-long panel at the 19th Annual Clinical meeting of the AAPM on “The Chronic Pain Experience.”
- Dr. Gildston also gave a presentation at that meeting on “Shifting the ‘noise’ of chronic pain to the background,” explaining how various psychological interventions in the areas of Complementary and Alternative Medicine (CAM) can significantly ameliorate chronic pain.
SLEEP DISORDERS
We treat all sleep disorders except sleep apnea which requires a medical lab facility.
- Challenges:
- Difficulty falling asleep
- Light or troubled sleep
- Awakening too early
- Inability to go back to sleep after awakening (to go to the bathroom, for example)
- Fear of falling asleep
- Anxiety about not being able to fall asleep
- Nightmares/provocative or disturbing dreams
- Intervention Techniques:

ANXIETY & DEPRESSION:
Dr. Gildston: Professional Member: Anxiety and Depression Association of America; American Psychological Association; American Counseling Association; Association of Spirituality and Psychotherapy; Association for Psychological Science; American Psychoanalytic Association-Psychotherapist Associate; Diplomate APA; Fellow, NAMA
Anxiety Disorders:
Have you ever felt any of the following sensations?
- restless or a sense of edginess
- easily tired
- can’t concentrate
- wondering if your mind is going "blank"
- irritable
- muscle tension
- can’t fall asleep or stay asleep

Or even more worrisome:
- Are you avoiding people, places, or situations that are reminiscent of a traumatic event?
- Do you re-experience some trauma in repeated nightmares or flashbacks?
- Is it difficult for you to trust others?
- Are you paying too much attention to staying safe or keeping loved ones safe?
- Do you startle easily?
- Are you struggling with a sense of a bleak or foreshortened future?

Perhaps you have even experienced the far end of the anxiety spectrum:
- palpitations?
- chest pain, chest tightness, feeling like you may be having a heart attack?
- shortness of breath or trouble breathing?
- sweating of the palms?
- nausea or other stomach upset?
- trembling or shaking?
- dizziness, unsteadyness, lightheaded, or faint?
- feelings of unreality or feeling detached from yourself?
- fear of losing control or going insane?
- numbness or unexplained tingling sensations?
- chills or hot flashes not related to anything physical?
- feeling like you are choking?
- sensing impending doom?
- feeling like you are dying.
Just imagine what it would be like if you were able to conquer these demons. We’ve helped many a patient do just that using many of the therapeutic techniques described above. Click on the links below to learn more:
Dr. Gildston has conducted the following workshops on Anxiety Disorders:
- “Breathing, thinking, and anxiety.”
- “Post-traumatic stress in our veterans.”
- “The OCD non-cure.”
- “Anxiety related to physical pain CAN be diminished.”
- “How to overcome public speaking phobias”

Dr. Gildston co-authored (with her late husband) the following article:
"The Hidden Message in Crisis Related Stress.” (Abstract) in Program and Abstracts, Third International Conference on Psychology, Stress and Adjustment in Time of War and Peace, Tel Aviv: Tel Aviv University, 1983, 138.
Please note that although Obsessive Compulsive Disorder (OCD) is considered by the DSM to be an Anxiety Disorder, there is considerable evidence that it differs significantly from other anxiety disorders. Hence we have added a special section for OCD just below this section on Anxiety & Depression.
Depression:
Some symptoms of depression overlap with those of anxiety. Some are more unique. Many of you may be struggling with both disorders. Imagine what it would be like if you could minimize or eliminate some of the emotional downers listed below. If so, consider coming to our center where we have been helping patients see the glass not only half full—instead of half or fully empty—but actually moving toward the top.
- feelings of low self-worth
- heightened self-depreciation
- a sense of guilt
- deep sadness
- hopeless
- pessimistic
- loss of capacity to take pleasure in day to day activities
- reduced energy
- slowed down thinking
- slow to act upon needs
- loss of appetite
- sleep problems

One of the most common psychological complaints, depression varies in reasons for onset, severity, and pattern of occurrence from one person to another. It is twice as prevalent in women.
Some believe that a major component may be defective regulation of one or more naturally occurring neurotransmitters, particularly norepinephrine and serotonin. Hence medication is often prescribed to rebalance these neurotransmitters. Typically medications provide help but too often improvements are only temporary for some.
There is also research that has found a connection among depression, disordered REM sleep, and changes in the amygdala, the center of emotions in our brains. In refractory cases more dramatic methodologies have been used, including electroconvulsive therapy (ECT), gene therapy, and deep brain stimulation (DBS). These more experimental approaches are associated with potentially serious side effects.
Research indicates that some form of psychotherapy—with or without medication—is crucial for effecting more permanent changes for the better. Typically such medications provide help but too often improvements are only temporary for some patients.
Dr. Gildston has conducted the following workshops on Depression, among others:
- “Singing the blues or having the blues?”
- “Hope for the down and out”
- “Depression, bipolar, borderline: How clear are the boundaries?”
AUTISM SPECTRUM DISORDER (ASD) & SENSORY PROCESSING DISORDER (SPD)
When Dr. Gildston served as Professor at Brooklyn College, she was the Director of the Diagnostic Laboratory. She supervised the diagnosis of autism and sensory processing disorder, among many other disorders. One of her four licenses: Speech/Language Pathologist.
Autism Spectrum Disorder (ASD):
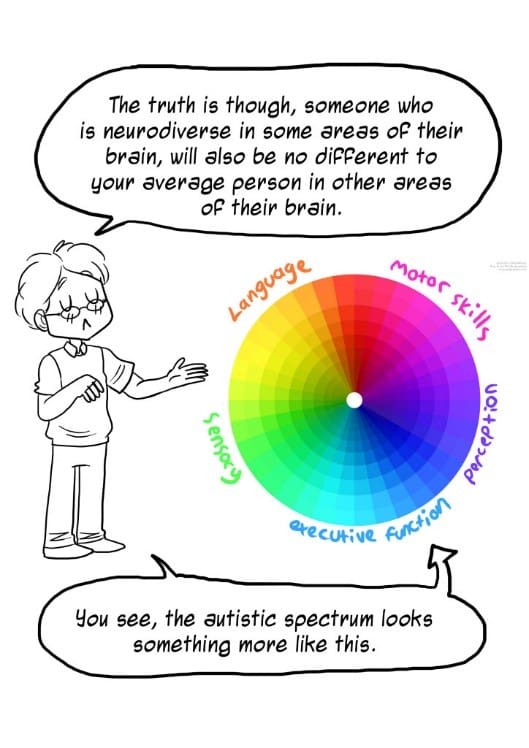
Challenges:
Persistent challenges across multiple contexts in:
- Social Communication: awkward back & forth talk; deficits in sharing imaginative play.
- Social Interaction: reduced sharing of interests, emotions, or affect; little need to keep or establish friendships.
- Non-optimal integration of verbal & non-verbal communication.
- Sometimes: abnormal eye contact &/or body language; repetitive motor movements; insistence on sameness; restricted fixed interests.
- Deficits in using or reading gestures.
- Hyper-or hypo-reactivity to sensory input: sound sensitivity, light fixation, excessive smelling or touching objects, and the like
Sensory Processing Disorder (SPD):
Sensory Processing Disorder (SPD) Sensory information goes into the brain but does not always get organized into appropriate responses considering the context. Although there is no damage to the sensory systems (such as blindness or deafness), sensory input from one’s body or the environment is poorly detected, modulated or interpreted. It has sometimes been described as a neurological “traffic jam” preventing parts of the brain from receiving needed information to interpret sensory information correctly.

OBSESSIVE COMPULSIVE DISORDER (OCD):
Do you have morbidly recurring thoughts that are incompatible with your self-image? Do they lead you to perform ritualistic acts in order to get temporary relief from such thoughts that go round and around? Are you disturbed or ashamed of your thoughts and actions but unable to cease and desist? If so you are probably suffering from a fairly common disorder called Obsessive-Compulsive Disorder. OCD ranges from relatively unclear, rather vague obsessions to highly specific recurring thoughts with or without observable accompanying compulsions. The scope of possible obsessions is vast, from cycling images of you or a loved one dying in some horrible fashion to seeing filth on every object in sight—followed by a need to wipe each clean. You may have obsessions without overt compulsions but with covert thought compulsions.

Your OCD may be causing you so much stress and anxiety you have become depressed. Now you have a triple whammy to contend with: OCD, anxiety, and depression. You may sense your quality of life has gone downhill even though you may be able to function at work and in day to day activities. On the other hand, your compulsions could be interfering with your ability to work or get things done around the house.
We specialize in helping you handle these unfair challenges in your life.
Alternatively, have your parents, friends, or spouse been upset with your “weird” rituals and tried to persuade you to stop or limit them? Perhaps you don’t understand why they are making such a fuss over some of your thoughts and actions. Indeed, they may seem perfectly reasonable to you and in tune with your self-concept. You may even derive pleasure from doing what others find objectionable. If this overview describes you, you may (or may not) have what has been labeled Obsessive-Compulsive Personality Disorder. In that case, you may not wish to change. If you are a parent, friend, or spouse of someone who fits this category, you may come to us to learn how you may motivate your friend or loved one to seek professional help.
- Challenges:
- Sexual Images
- Incest
- Rape
- Animal
- Genitals
- Homosexual
- Heterosexual
- Religious Images
- Cleanliness & Washing
- Death & Dying
- Counting
- Aggressive Acts
- Repeated Checking on Actions
- Movement Stereotypes
- …and more...
- Sexual Images
- Intervention Techniques:
- Cognitive Behavioral Therapy (CBT)
- ERP (Exposure Ritual/Response Prevention
- Prolonged Exposure Therapy
- Exposure Therapy
- Hypnotherapy & Guided Imagery
- Art Therapy
- And more….
- Cognitive Behavioral Therapy (CBT)
- The following may be OCD symptoms or just bad habits:
- Skin Picking
- Hair or Eyebrow Plucking
- Nail Biting
- Throat Clearing
NB: CBT and the variants above (especially ERP) have been proven to be the most effective approaches for relieving OCD symptoms. Other approaches are add-ons which may help to minimize the anxiety and hopelessness that often accompany OCD.

Our Director, Dr. Gildston, has chaired and taken part in several workshops on OCD including:
- “Whirling thoughts: the opposite result from that for whirling dervishes.”
- “Does ERP really work?”
- “The debate on whether OCD can be cured.”
- “How clean is your OCD clean?”
- “Santa Claus is only checking it twice.”
- “Covert obsessions may produce covert compulsions.”
SUBSTANCE ABUSE ADDICTIONS:
Dr. Gildston: Professional Member, National Association of Alcohol and Drug Abuse Counselors (NAADAC); DOT Certified Substance Abuse Professional (SAP); Certified Professional Member, Feeling State Addiction Protocol (FSAP)
Have you been struggling with one or more substances? Do you feel like the substance is in control rather than you?
If you’re looking at this website there’s probably a part of you that may want to reign in some of these abusive or addictive behaviors. You may want to find a new way to live calmly in the present as well as to look forward to a more positive and in-control future.
For 25 years we have worked with adults and teen-agers with these problems—individuals like you who want to make significant changes in their lives. All of us are licensed PhD doctors who are broadly trained. We specialize in alternative, totally drug-free rehabilitation techniques. We decide together with you which intervention(s) will be best for you. For those of you with multiple abuses or addictions, know that we only work on those substances which you have elected to conquer.

-
Challenges:
-
-
Alcohol
-
Cocaine
-
Heroin
-
Marijuana
-
Nicotine
-
Uppers
-
Downers
-
-
- Vicodin
- Neurontin
- Meth
- Ecstasy
- LSD
- ... and all other legal and illegal addictive substances
- Co-Morbidities:
- Intervention Techniques:
-
- Art Therapy
- Dream Work
- Biofeedback
- …and more
Our Director, Dr. Gildston, has presented several workshops on Substance Abuse & Addictions including
- “Differing approaches to the treatment of substance abuse and addiction.”
- “A treatment attack on recidivism in addiction.”
- Presented a workshop entitled “Eating Disorders and Substance Abuse: Prevention and treatment for a spectrum of artful and dangerous addictions” at the 2009 Annual Conference of the NAADAC, the association for addiction professionals.
ADDICTIONS AND COMPULSIVE BEHAVIORS:
Compulsive Activities: (Must be differentiated from Obsessive Compulsive Disorder.)
Do you have an activity interest that has taken over your life? If you’re truly happy in that pursuit you don’t need our help. If, on the other hand, it has become a compulsion which is causing you significant interpersonal, family, and (or) personal grief—even though you may still be deriving pleasure from the activity—we can help you conquer that compulsion. We can even help motivate you to want to cease and desist. Our licensed PhD doctor specialists have been doing so for 25 years.
For 25 years we have worked with adults and teen-agers with these problems—individuals like you who want to make significant changes in their lives. All of us are licensed PhD doctors who are broadly trained. We specialize in alternative, totally drug-free rehabilitation techniques. We decide together with you which intervention(s) will be best for you. For those of you with multiple abuses or addictions, know that we only work on those substances which you have elected to conquer. An example of one technique among many which we use to help free you of addictions is FSAP. In the words of its creator:
“Impulse-control disorders such as pathological gambling, sexual addiction, and compulsive shopping cause enormous suffering in people’s lives. The feeling-state theory of impulse-control disorders postulates that these disorders are created when intense positive feelings become linked with specific behaviors. The effect of this linkage is that, to generate the same feeling, the person compulsively reenacts the behavior related to that original positive-feeling event, even if detrimental to his or her own wellbeing. This reenactment creates the impulse-control disorder. The therapy described in this article is the Impulse-Control Disorder Protocol (ICDP), which uses a modified form of eye movement desensitization and reprocessing (EMDR) to address these fixations.
- Identify the exact behavior that has the most intense positive feeling.
- Identify the exact feeling that underlies that behavior.
- A modified form of EMDR is utilized to break the connection between the feeling and behavior.
- The negative beliefs that underlie the compulsive fixation are processed.
- Challenges:
-
- Compulsive Gambling
- Racing
- Poker
- Slot Machines
- Casino Board Games
- Stock Market
- ... and the like
- Compulsive Gambling
-
- Compulsive Shopping
- Compulsive Internet Surfing
- Extreme Sexual Excesses
- Pornography Excesses
- Overworking
- Overeating

- Intervention Techniques: (See Substance Abuse Addictions above)
- There is a new technique—an off-shoot of EMDR —called Feeling State Addiction Protocol (FSAP) which has had some excellent results in eliminating addictions:
FSAP: Dr Gildston is Certified in FSAP
-
- Any feeling can become fixated with any behavior.
- Identify the exact feeling & the exact behavior.
-
- Look for the most intense positive feeling connected with the compulsive fixation.
- Process the fixation with a modified form of EMDR.

Per the creator or FSAP, an addiction can be triggered by either an internal or external event. Hence:
Intense Desired Feeling + Positive Event = Addictive Fixation
OR
Addictive Fixation + Trigger Event = Addictive Behavior
The FSAP breaks the fixation between feeling and behavior. Once this connection is broken, there are no cravings or urges to be controlled, no behavior to be managed.


Embarrassing Bad Habits & BFRB:
Do you have a bad habit that is causing you embarrassment, annoyance, or problems with friends and loved ones? You do NOT have to continue living with it. You CAN conquer it with our help.


- Challenges:
- Skin Picking
- Hair Pulling
- Nail Biting
- Nose Picking
- Repetitive body movements
- Excessive procrastination
- Compulsive lateness
- Extreme Cluttering
The TLC Foundation for Body-Focused Repetitive Behaviors (BFRB) states the following:
“Body-focused repetitive behaviors may include any repetitive self-grooming behavior that involves biting, pulling, picking, or scraping one’s own hair, skin, or nails that results in damage to the body. While most people engage in one or some of these behaviors to a certain degree, an individual may want to seek help and support if the behavior begins to limit their life in some way, feels out of control, causes physical damage, or is causing social impact. …the symptoms must cause clinically significant distress or impairment in an area of daily functioning and cannot be better explained by stereotypic movement disorder or non-suicidal self-injury.”
Dr. Gildston is a professional member of The TLC Foundation for Body-Focused Repetitive Behaviors.
- Technical Terms:
- Onychophagia
- Onychotillomania
- Trichophagia
- Dermatophagia
- Lip Bite Keratosis
- Cheek Keratosis
- Tongue Chewing
- Trichotemnomania
- & More
- Intervention Techniques: (See Substance Abuse & Addiction above)
Compelling Consumables:
Even though your weight may remain unchanged and you may have no diagnosable eating disorder, do you compulsively consume excessive amounts of junk food? We can help you conquer this extremely unhealthy compulsion.
- Challenges:
- Excessive Consumption of Caffeine (Coffee, Chocolate, Caffeinated Soft Drinks, etc.)
- Excessive Consumption of Sugar (Cakes, Cookies, Candy, soft Drinks, etc.)
- Excessive Consumption of Junk Foods (Excess Trans-fats, Sugar, Salt, etc.)
- Excessive Consumption of Chemically Altered Foods (Foods with Multiple Additives)


- Intervention Techniques: (See Substance Abuse & Addiction above)
SELF DEFEATING ATTITUDES:
Self Defeating Negativity:
Have you turned friends and family off with an excessively negative attitude? If you’re satisfied—even happy—with such consequences, you would certainly not be looking at this website with a desire to change. But if you believe you might be more content by becoming more positive, we can definitely help.
- Challeges:
- Hypercritical of others
- Excessively complaining
- Excessively confrontational
- Excessively aggressive

Self Defeating Avoidance:
On the other hand, you may have been behaving in ways that attempt to disguise who you really are because you are insecure or think ill of yourself. If that is the case, you’re probably NOT particularly happy or content. We can help you become more interpersonally courageous and more self-accepting.

- Challenges:
- Excessive people pleasing
- Totally non-confrontational
- Insecure or shy with the opposite sex
- Passively aggressive
- Socially anxious or avoidant
- Anxious when speaking publicly or performing
Anger Management
Dr. Gildston: Professional Member and Fellow, National Anger Management Association.

- Challenges:
- Excessively angry
- Outbursts of rage
- Temper tantrums
- Verbally abusive
- Tendency to engage at times in physical abuse
- Intervention Techniques: (See Counseling and Psychotherapy above)
SELF-ESTEEM ISSUES
Do you hear yourself repeatedly saying to yourself negative comments such as:


If so, you probably know, consciously or at a gut level, that you have a significant self-esteem issue. Unfortunately, a poor self-image can potentially lead to a host of disturbing sequelae:
- Loneliness
- Anxiety
- Fear
- Despair
- OCD/Addictions
- Workaholic Behavior
- Depression
- Embarrassment
- Shame
- Panic Attacks
- Sexual Dysfunction
- Boundary Issues
- Distorted Body Image (BDD)
- Hypersensitivity/Hypervigilance
- Underdeveloped Social Skills
- Unrealistic Expectation
- Over/Under Achiever
- Lack of Assertiveness
EVEN: Self-hate or Self-harm
We offer multiple interventions (see our extensive list of psychological approaches) to help you reverse these negative self-accusations which, in turn, allows their negative consequences to recede significantly. Our goal is to move you toward a sense of psychological strength and belongingness as well as toward a capacity for making more rational evaluations of outcomes. We aim for you to progress toward a realistic measure of self-love.
Our Director, Dr. Gildston, has run workshops on the following related topics:
- “The PLEASER: child to grandma: symptoms & solutions.”
- “Understanding self-harm, from self-slapping to cutting.”
- “How to be alone and not feel lonely.
- “I shoulda, woulda, coulda, but didn’t !”
STRESS MANAGEMENT:
Personal & Family:
If you can't handle stress you may adversely affect your health and your sense of well-being. In response to both internal and external stresses, shifting moods may turn others off. Relationships may be endangered. Stresses related to work, family, friends, and lovers are addressed.
- Techniques for reducing stress are taught, including:
-
- Meditation
- Self-hypnosis
-
- Cognitive-behavioral shifts
- Changes in patterns of verbal and non-verbal behavior
-
- .....and more
Corporate:
To improve morale and thereby increase output efficiency, we evaluate, analyze, report on, and teach how to minimize interpersonal stresses and conflicts within and between:
- Individuals within departments
- Different departments
- Hierarchical ranks from the highest administrative to the new working recruit levels
For example, a supervisor may be unaware that when he purposefully or unconsciously intimidates a worker, he is likely to impede the worker's productivity or creativity. On the other hand, the worker may not know how to cope effectively with such abuse.
Group programs are customized to reduce stress and create harmony. Thereby such programs enhance morale and increase productivity.
POST TRAMATIC STRESS DISORDER (PTSD)/TRAUMA
Have you experienced…
-
- Sudden death or desertion by a loved one
- Mutilating car accident
- Severe abuse or neglect by a partner
- Violent criminal assault
- Military combat
- Life-threatening natural disaster
- Rape
- Critical child abuse, neglect, or abandonment
- Traumatic loss of a pet
- Observation of momentous traumatic event

Typically, the victim is unprepared for these events. Nor can she do anything to prevent the trauma since it is unexpected. The immediate response is one of helplessness, intense fear, and horror.
It’s possible you experienced one or more of these traumas but were able to rise like a phoenix out of the ashes. Your resilience may have been supported by an understanding family or friends. Perhaps a short bout of therapy was all that you needed or is what you need right now if you’re still experiencing some fear or anxiety about the event.
On the other hand, you may need serious therapeutic attention for unmitigating flashbacks, depression, suicidal ideation, hypervigilance, severe anxiety, or other self-defeating emotions. Perhaps you have some of the following symptoms because of negative pre-event, post-event, or actual event factors such as the following:
Negative Pre-event and Post-Event Factors
- Unstable familial or marital environment
- Previous exposure to child abuse or other traumas
- Absence of social support
- Poor coping skills or self devaluation
- Medical issues that complicate recovery
- Self-Pity leading to passive rather than active responses

Negative Event Factors
- The existence of an on-going threat
- Prolonged exposure with geographic nearness
- Profound meaningfulness of event for you


Intervention Techniques:
- Eye Movement Desensitization and Reprocessing (EMDR)
- Cognitive Behavioral Therapy (CBT) plus ACT, DBT
- Psychodynamic Psychotherapy
- Somatic Experiencing
- Clinical Hypnotherapy
- Exposure and Response Prevention
- Feeling-State Addiction Protocol (FSAP), PTT, & IRT
- Substance Abuse Therapy
(If you’ve tried escaping with drugs or alcohol)
In therapy you can increase your sense of coherence, develop an internal locus of control, increase self-efficacy, and improve both your physical and emotional strength by developing strong motivation to deal with the trauma and enhancing your optimism for change.
Our Director, Dr. Gildston, is certified at the most advanced level in EMDR, CBT, Clinical Hypnotherapy, and more. She is also a certified Substance Abuse Professional (SAP). Come for a free consultation.

